Hacking diabetes monitoring – can we do better?
Today, I’m going to take a different path, and invite entrepreneurs and innovators to contact me with their business ideas, and to start conversations on how we might develop them together. The subject area is digital healthcare monitoring.
This post is inspired by a brush with regulations here in the UK, and conversations with some friends about new ways to manage long-term conditions. Thanks are particularly due to Dr Nick van Terheyden for kicking this into action.
The problem
Here’s the context – here in the UK, type 1 diabetics fall under the declared medical conditions of the Drivers Medical Group at the DVLA. I fall under their remit, and have been fortunate to manage the condition pretty well for more than half a century. Last week, I renewed my driving licence, which is a requirement every three years, and follows a process of medical enquiries to determine continuing fitness to drive.
The process is efficient, but reveals a gap between the baseline view of the authorities on driving with diabetes, and the potential gains from emerging technology solutions. For diabetic drivers, much of the government paperwork talks about recognising the sensations of low blood sugar, and stresses the requirement not to drive under such conditions. They give guidance on testing blood glucose (BG) before a journey, and advise a minimum two-hour re-test frequency once the journey is in progress. Most diabetic patients will tell you that a lot can happen in two hours, and without frequent testing we are back to the patient’s ability to recognise sensations, and respond to them.
How I do things today
I have been privileged to have access to some neat technologies that have helped my management of the condition, and keep me well. My current solution is a bit of a technology hack, but crucially, offers a digital readout of blood sugar level, every five minutes, on the dash of my car. This is so valuable, as I can see trends as they happen, and prevent low BG events, rather than wait to feel the sensations and react after the fact. This gives me greater assurance of my fitness to drive, and is healthier, as over-correction is avoided, and BG stays within the target range.
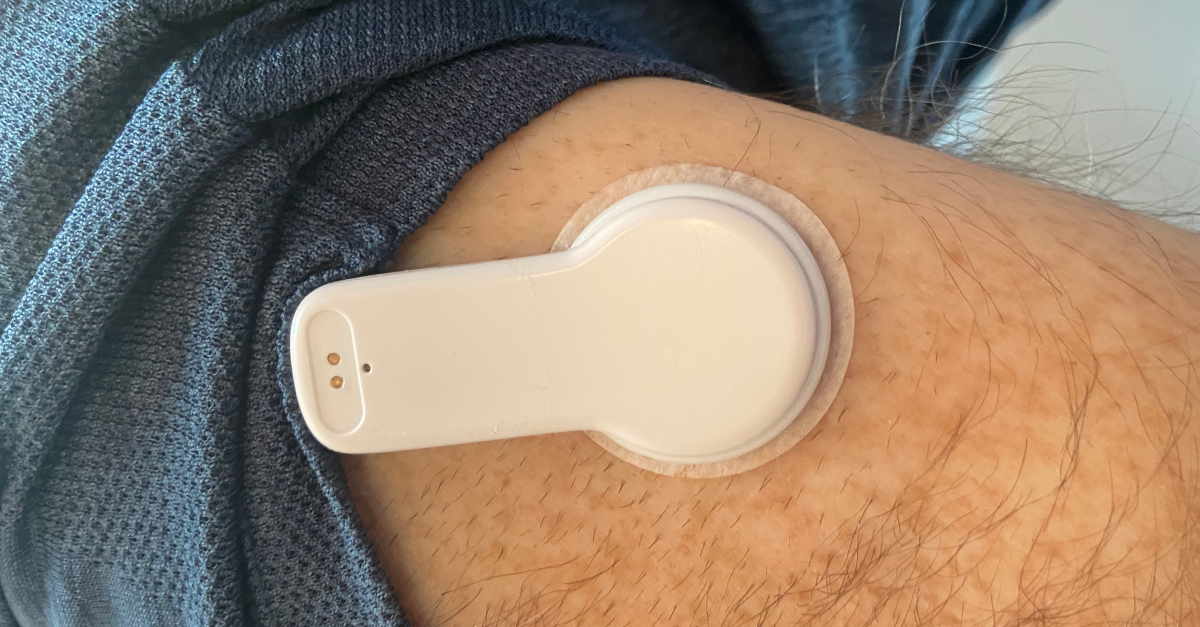

My personal rig combines different pieces of prescribed and commercially available equipment and software. It’s fragmented, and I’m aware that if one part no longer integrates with another, then the whole thing fails to deliver the intended benefits. This is the stimulus to look for better solutions.
I’ve been using Abbott’s Freestyle Libre for a few years now and it has been a revelation. These devices are coming more into general use, and are available in some cases on prescription from a GP, which is a welcome move. The device is a disk, about the size of a £2 coin, stuck to the rear of the upper arm with a small filament under the skin to sense the fluid there. It is read by scanning it with a reader, either provided by Abbott, or more conveniently, a suitably equipped mobile phone. All good so far, but this is not very convenient when driving, particularly considering the regulations on hand-held mobile phones in cars.
Enter the next discovery, called a MiaoMiao transmitter. I use version 2 of the device, which is about the same depth as the Libre sensor and is fixed to the skin and sensor with adhesive patches. It’s not too bulky and once set up (that’s a whole new chapter yet to write) works well. It needs a separate app on the iPhone – I use xDrip4iO5 but there are others that do a similar job on iOS or Android.
Best of all, it can use a workaround to export the BG reading as a short calendar event. This is the trick that lets the Apple Watch display readings for ease of tracking in everyday activities. New calendar events every five minutes show the value, trend and numerical change from the last reading. In the image it shows that four minutes ago, BG was 5.4 mmol/l, and had fallen 0.2 in the five minutes prior to that (the target range is generally accepted as between 3.9 and 10 mmol/l). That insight is priceless because if rapid change is happening, particularly if BG is falling, then a quick response can prevent hypoglycaemia, a low blood sugar event that can be dangerous if it’s not treated quickly.
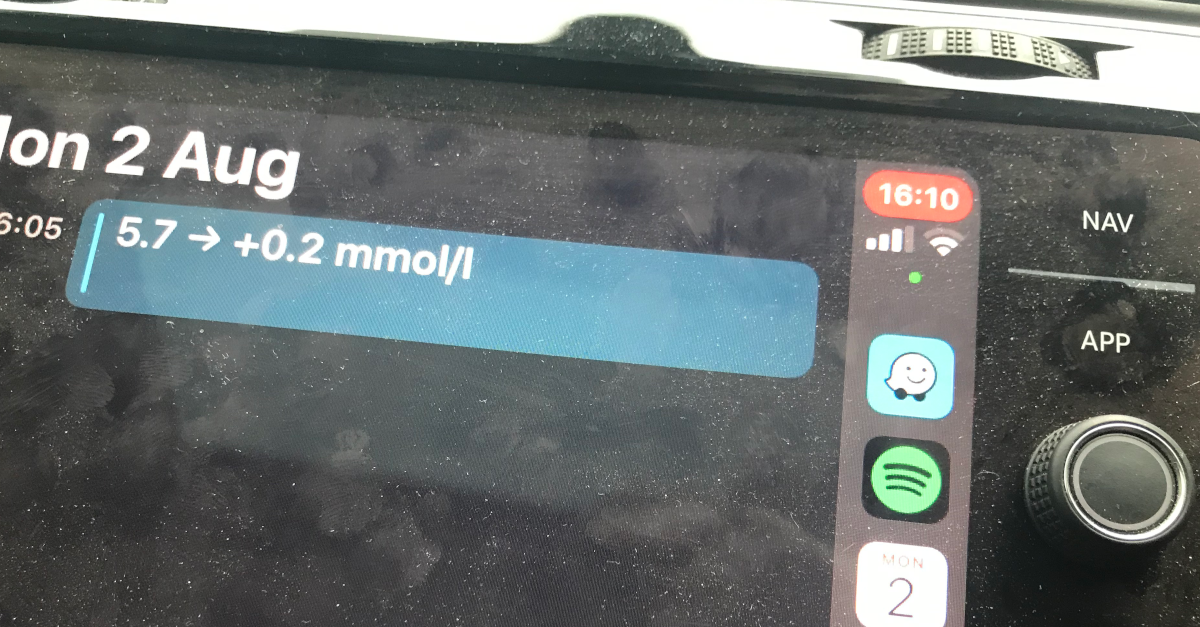
In the car, and with the right technology, it gets even better. My car has Apple CarPlay, with which I can see calendar items on the screen. As with the watch, every five minutes I can see my BG, and if it is starting to move then I can do something about it. In this example I can see that a few minutes after the watch reading, I am still fluctuating around the 5.5 level, and so in pretty good shape.
That has been the biggest single change in removing the guesswork on long journeys. Before this I would often play safety first, and eat snacks during the trip that would send me into high BG territory, which takes a long time to correct with additional insulin once the journey is over.
Is there a better way?
My arrangement is a lash-up with five different suppliers in the chain.
It relies on my use and experience with Abbott’s Freestyle Libre as the primary sensor. Of course, other CGM (Continuous Glucose Monitoring) systems are out there, but I have no personal experience with Dexcom, Eversense or the even deeper pool of sensors related to insulin pumps like MiniMed, so please let me know if I have missed a trick on any of those paths.
All that considered, here is my call. If there are entrepreneurs or healthtec innovators out there working on ideas to streamline the information chains to inform diabetic patients simply, and in real, or near-real time, I’d love to hear from you. There must be a more joined-up solution that is less vulnerable to compatibility or interface issues, and will deliver reliable insight for mobile diabetics. Sensing and monitoring like this is not unique to diabetes, but it is my starting point. I think there is a big future, and lots of value, in wearable sensing technology coupled with data and analytics to improve awareness and management of chronic conditions.



Diabetes Hacking for Drivers - Dr Nick
May 16, 2022 @ 10:09 am
[…] the US and almost half a million in the UK) it is highly significant – you can read all about Phil’s Diabetes Driving Hack here that cobbles together a host of wearable technology and add on devices to create a drivers alert […]